If you need help managing a brain or spine condition, turn to the specialists at Valley. Our team routinely helps people who:
- Have a serious medical condition, such as a brain tumor, that requires neurosurgery or Gamma Knife radiosurgery
- Have a painful back problem, such as spinal stenosis, that requires spine surgery
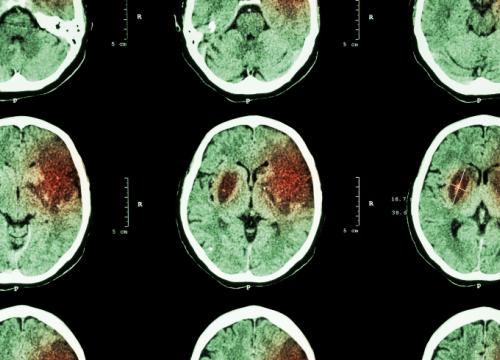
- Had (or are at risk of having) a stroke or brain aneurysm
- Have new or worsening neurological symptoms such as pain, numbness, tingling, and weakness
- Need help managing a chronic condition, such as epilepsy or Parkinson’s disease
- Are looking for a second opinion about their treatment options
Because we offer the same level of expertise as many larger medical centers, you don’t have to travel as far to get the care and support you need to live well with your condition — or overcome it.
The Valley Approach to Brain and Spine Care
No matter what type of neurological or neurosurgical care you need, you can count on Valley for a caring, personalized experience.
Our team members — including neurologists, brain surgeons, spine surgeons and endovascular neurosurgeons — start by getting to know you. We take the time to understand how your symptoms or condition affect your ability to work, play and take care of yourself or others. We also spend time answering your questions, addressing your concerns and explaining the benefits and risks of different therapies.
This approach to brain and spine care help us create a treatment plan that’s safe and effective but also aligns with your personal goals and preferences. In some cases, we can identify a less invasive treatment option.
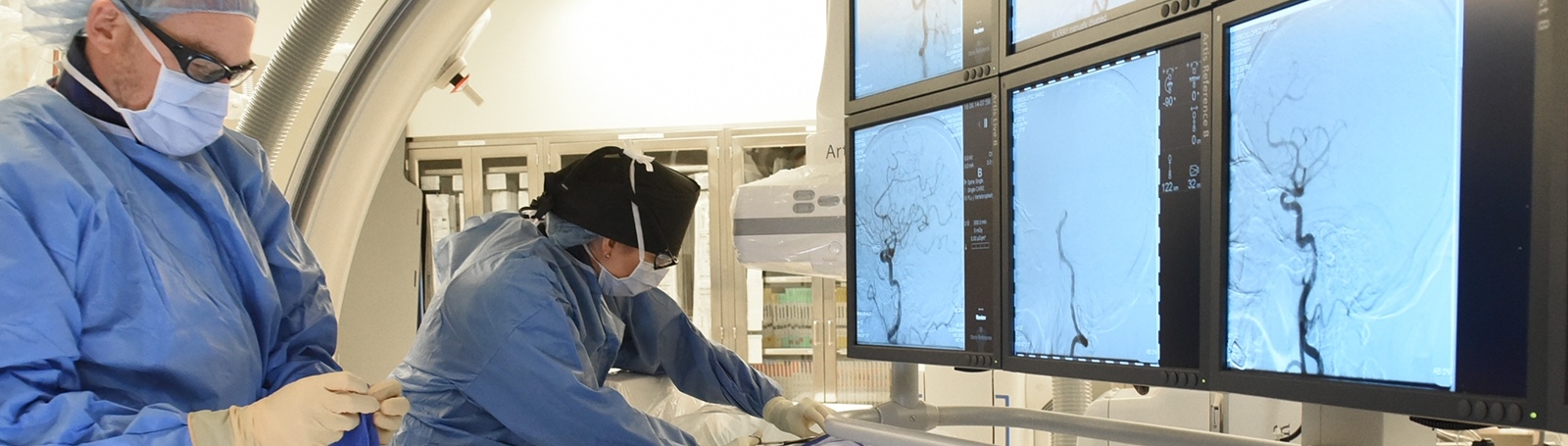
Should you need brain surgery or spine surgery, you can take comfort knowing our neurosurgeons have extensive training and experience. In fact, our endovascular neurosurgeons offer the latest minimally invasive treatments for blood vessel problems in or near the brain (cerebrovascular disease). These techniques let us treat stroke, brain aneurysm and other life-threatening conditions without having to make large surgical incisions.
Our Areas of Care
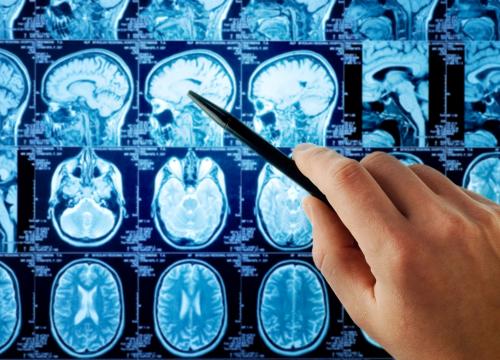
Neurology
Because many of our neurologists specialize in specific conditions, you can rest assured you’re getting the highest level of care available. Our areas of expertise include:
Brain Surgery
Brain surgeons at Valley have experience treating serious or life-threatening neurological conditions. These include:
Spine Surgery
Our spine surgeons offer advanced treatments, including the latest minimally invasive procedures, for common and complex spine conditions. These include:
- Herniated discs
- Scoliosis
- Spinal Stenosis
- Spinal Tumors
Endovascular Neurosurgery
New, minimally invasive treatments available at Valley let us treat many cerebrovascular problems. These include:
- Brain Aneurysm
- Pulsatile Tinnitus
- Pseudotumor Cerebri
- Stroke
Why Choose Valley for Brain and Spine Care?
- Complete care, close to home: When you receive brain or spine care at Valley, you have access to a broad range of local services that support your ongoing treatments or recovery. These services include rehabilitation, home care, pain management, brain cancer care and more.
- The gold standard of stroke care: The Valley Hospital has been designated a Comprehensive Stroke Center — the highest honor a hospital can achieve — by The Joint Commission. This means patients brought to our emergency room have access to the most advanced stroke care available, including minimally invasive procedures that give you a better chance of survival and recovery.
- Advanced brain aneurysm care: We offer the full range of treatments for ruptured and unruptured brain aneurysms, including minimally invasive procedures that aren’t widely available. In addition to performing traditional surgery (aneurysm clipping), our specialists can choose from several endovascular procedures. Because we offer various options — including aneurysm coiling, flow diverter stents and WEB aneurysm treatment — we can tailor your treatment to the size, type and location of your aneurysm.
- Unmatched support: Finding out you need medical treatment for a brain or spine condition can be scary, but you don’t have to go through this alone. If you need help understanding your diagnosis or treatment options, or have questions about support services, you can count on Valley’s neuroscience nurse navigator for one-on-one guidance at every turn.
- Neuroscience intensive care unit (ICU): Our neuroscience ICU is reserved for patients hospitalized with a serious neurological illness such as a stroke, or those recovering from brain surgery or endovascular neurosurgery. This unit is comprised of private rooms and is staffed by doctors, nurses and other providers with advanced training in critical care and neurological disorders.
- Outstanding cerebrovascular outcomes: To help improve treatment options for patients with cerebrovascular disease, Valley participates in the national NeuroVascular Quality Initiative-Quality Outcomes Database (NVQI-QOD). This database tracks outcomes for each endovascular neurosurgery procedure we (and other participating hospitals) perform. Our data confirm we continuously meet or exceed strict clinical criteria related to patient safety and quality, including average length of stay in the hospital, complication rates and more.