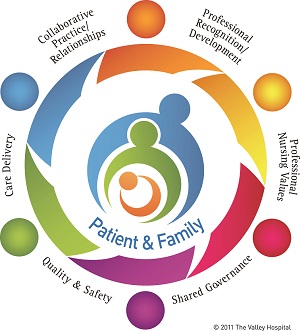
 Nursing at The Valley Hospital is grounded in our Professional Practice Model (PPM), which is based, in part, on the work of nursing theorist Dr. Jean Watson. Our PPM guides our nurses as they provide quality care to patients and their families, collaborate with interdisciplinary teams, and contribute to the profession of nursing.
Nursing at The Valley Hospital is grounded in our Professional Practice Model (PPM), which is based, in part, on the work of nursing theorist Dr. Jean Watson. Our PPM guides our nurses as they provide quality care to patients and their families, collaborate with interdisciplinary teams, and contribute to the profession of nursing.
Each section in the model highlights the essential domains of nursing practice at Valley. All domains encircle the center, emphasizing that the patient and family are at the center of all that we do.
Professional Recognition/Development
The Valley Hospital values, encourages, supports and recognizes professional development and believes this is a part of the foundation of nursing’s commitment to continued excellence. Professional recognition and development is important to Valley nurses and is a necessary ingredient to ensure a competent nursing workforce. A part of nursing’s vision statement is to have a professional practice environment that attracts and retains highly qualified nurses, and part of nursing’s philosophy is a commitment to professional development through lifelong learning.
Professional Nursing Values
The role of the registered nurse (RN) is unique and essential to care of the patient. The RN possesses nursing knowledge, skills and judgment that can only be acquired through an approved nursing program. Nurses are the only healthcare providers at the frontline of patient care delivery around the clock and are required to be knowledgeable about acute and chronic diseases, medication management, ethical decision-making, effective communication, patient education, cost-benefit analysis and complex technologies, to name a few. The RN is accountable and responsible for the provision and coordination of care for an assigned group of patients, which includes assessment, planning, intervention and evaluation. The tenets within professional nursing values are core to our practice.
Shared Governance
The Magnet Recognition Program® provides the foundational framework for nursing excellence. It provides guidelines for structures and processes to be developed, disseminated and enculturated for all levels of nursing wherever nursing is practiced. Shared governance is defined as a dynamic nurse-nurse leader partnership that promotes collaboration, shared decision-making, and accountability for improving quality of care, safety and enhancing work life. It embodies four principles: partnership, accountability, equity and ownership.
In order to support shared governance, nurse leadership demonstrates a commitment to empowering the direct-care nurse and sharing authority with regard to RN professional practice. Direct-care nurses are treated as partners and team members, understanding that their personal goals are in alignment with accomplishing the mission and goals of nursing and the organization. Nursing leaders at Valley must possess the characteristics of a coach, mentor, role model, facilitator, coordinator, integrator and teacher.
Quality
The Valley Hospital nurses fulfill the role of professionals, which requires being highly skilled, highly motivated, committed to quality and fully engaged in the professional practice of nursing. As each nurse continues to evolve his/her professional potential, the results of open communication, participation in governance activities, and pursuing advancement of knowledge and skills lead to the continual strengthening of our mission and values.
Care Delivery
Our care delivery system/model flows from our PPM, which reflects our commitment to placing the patient and his/her family at the center of all that we do. This patient- and family-centered focus is the foundation of our nursing care delivery model, which incorporates patients and their family members as true collaborative partners in care.
Collaborative Practice/Relationships
By developing solid collaborative partnerships, we foster an environment in which all professional healthcare disciplines can work together to meet the goals of the patient, patient care departments, division leadership and the organization. Key to collaborative relationships is the collegiality between nurses, physicians, leadership, ancillary patient care staff and the entire healthcare team. Through our structure and processes, we are able to continually improve nursing outcomes and strengthen the interdisciplinary collaboration within the organization. Nurses play a collaborative and collegial role both in hospital operations and the delivery of patient care.

