Transcatheter aortic valve replacement (TAVR) is a minimally invasive procedure to replace the aortic valve. It is used to treat severe aortic stenosis (narrowing or blockage in the aortic valve).
TAVR is a less invasive approach than open-heart surgery to replace the aortic valve. This can mean less pain, faster healing and an easier recovery. It can be a life-changing option for people who are not candidates for heart surgery.
Valley’s structural heart specialists and heart surgeons have performed over 1,000 TAVR procedures. With any heart procedure, experience is important for the highest quality outcomes.
Am I a Candidate for TAVR?
If you have severe aortic stenosis, TAVR may be a good option for you. Your care team at Valley will discuss your options with you, as well as the risks and benefits of TAVR.
TAVR might be right for you if:
- You have medical conditions, such as a previous heart attack, that make open-heart surgery more risky
- You are too frail for open-heart surgery
- You have had a previous aortic valve replacement
The TAVR Procedure
A narrowed aortic valve can restrict the flow of blood from the heart to the body. It causes the heart to work harder and eventually leads to heart damage. If you have severe aortic stenosis, your primary treatment option is aortic valve replacement.
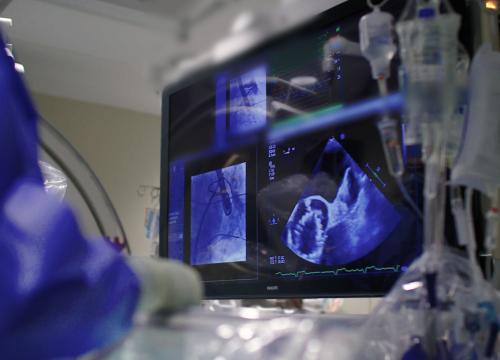
Heart surgeons and structural heart specialists at Valley work together to perform TAVR procedures. They start by inserting a catheter (a thin, flexible tube) through an artery in the groin or shoulder area.
The catheter carries the artificial replacement aortic valve through the blood vessels and to the heart. Once in place, the specialist inserts the valve inside the narrowed valve.
You will be sedated for the procedure to reduce any discomfort.
Recovery From TAVR
While TAVR is minimally invasive, it’s still a major heart procedure.
Compared to open-heart surgery, healing after TAVR is faster, and you’ll experience less pain and scarring.
You can expect to recover in a private hospital room for one to three days after the procedure. You should be able to walk around a few hours after surgery. About 80% of patients at Valley go home the next day after TAVR.
After you leave the hospital, you should be able to get back to normal activities, like driving, within a week of the procedure.
Why Choose Valley for TAVR?
- Expertise in valve repair and replacement: The Valley team has vast experience in TAVR. We’ve not only performed more than 1,000 procedures, but we also provide the full range of aortic valve surgeries. Additionally, we can offer you access to some of the most cutting-edge clinical device trials in the nation.
- Team-based decision-making: Our heart surgeons and structural heart specialists collaborate to plan and perform TAVR. As a team, we design the best approach for your specific condition. We’ll help you understand the procedure and what to expect every step of the way.
- Complete care for your aortic condition: Valley offers integrated aortic care for patients with aortic aneurysms. We also offer comprehensive care for complex valve conditions in our valve center. At Valley, multiple specialists are available to you, all with the goal of providing you with concierge-level service.
- Convenient, coordinated services from the very start: We schedule all the pre-procedure testing on the same day to make life a little easier for you. Our cardiovascular nurse practitioners will help you understand all aspects of TAVR and your recovery. And our nurse navigators will coordinate your appointments, making it easier for you to focus on your health.