NEW KNOWLEDGE, INNOVATIONS, AND IMPROVEMENTS focuses on how clinical and operational practices are based on research, evidence-based practice, and innovation.
Valley’s Heart Failure Team Successfully Implants First LVAD

Last year, Valley’s Center for Comprehensive Heart Failure Care team successfully implanted its first left ventricular assist device (LVAD) – a mechanical pump that supports heart function and blood flow in patients with advanced heart failure. The surgically implanted device supports patients whose hearts can no longer pump sufficient blood to meet their body's needs.
For individuals with end-stage heart failure, LVAD therapy offers several benefits over medical therapy alone, including improved organ function, symptom relief, enhanced physical activity, improved longevity and the opportunity for at-home recovery.
For patients who are able to recover at home, Valley’s heart failure care team has partnered with Valley Home Care (VHC) to provide post-operative care for LVAD patients and help prevent unnecessary rehospitalizations. Last year, Nancy Elmann, RN, MSN, CCRN, CHFN, VAD-C, NP-C, VAD Coordinator and Heart Failure APN, provided comprehensive training to VHC’s cardiac and IV nursing teams to ensure they were well versed in the specialized care required for LVAD management.
Through close collaboration with Nancy and the entire heart failure care team, VHC is able to provide safe, reliable care to LVAD patients in the comfort of their own homes.
By combining the latest innovations in heart failure treatment with the expertise of our highly skilled care teams, Valley looks forward to continuing to provide exceptional care to our cardiac patients.
Telephonic Assessments Keep Patients Safe at Home
In March 2025, Valley Home Care launched the Telephonic Care Management (TCM) program to help reduce unnecessary hospitalizations and improve the quality of life for high-risk patients being cared for in their homes.
With the support of two clinical coordinators and a health coach, the TCM program provides telephonic assessment and appropriate interventions to allow patients and their families to manage their condition(s) safely at home. Using the Pulse platform, the clinical coordinators – Elaine Davis, RN, and Rose Ranuro, RN, MSN, APN – proactively identify high-risk individuals (most commonly patients with congestive heart failure and chronic obstructive pulmonary disease) and invite them to participate in the program.
Once enrolled, patients receive check-in calls up to three times per week from Elaine and Rose. Through these conversations, they assess symptoms, review any trends in vital signs, and determine whether further action is needed, including whether a patient requires a nursing visit, medication adjustment, urgent assessment, or emergency care. When concerns arise, the coordinators collaborate closely with field nurses and primary case managers. They notify clinicians, communicate directly with physicians when necessary, and can coordinate urgent in-home evaluations through services such as DispatchHealth. By maintaining consistent communication and strong interdisciplinary collaboration, the program enhances continuity of care and supports timely, informed decision-making.
If patients lack essential equipment, such as a scale or blood pressure cuff, Janine Sedlak, Certified Health Coach, ensures those tools are provided. Janine also helps onboard patients to the TCM program and escalates clinical concerns to the clinical coordinator or case manager as needed.
Since its launch, the TCM program has maintained an average enrollment of 55 to 60 patients. Valley Home Care looks forward to continuing to grow the program in 2026 to help high-risk patients prevent avoidable hospitalizations while being safely cared for in their homes.
Lactation Team Launches Donor Breast Milk Program
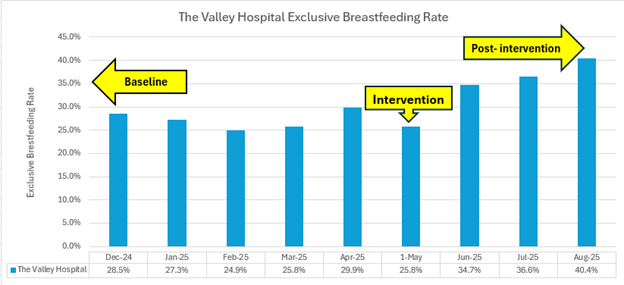
To help boost Valley’s exclusive breastfeeding rates for infants born at the Center for Childbirth, Valley’s Lactation Department implemented a new program in 2025 that offers parents complimentary donor breast milk for their infants in Postpartum and the NICU.
In response to declining rates, Katie Ver Hage, MSN, BSN, RNC-OB, C-EFM, IBCLC, Manager of Maternal-Fetal Medicine, Family Education and Lactation, and her team went back to the literature and found that supplementing through donor breast milk can provide a short-term “bridge” to breastfeeding, often improving long-term breastfeeding outcomes. The lactation team decided to partner with the Mothers’ Milk Bank of the Northeast and made their first purchase of three 100-mL bottles of donor milk in May 2025. Originally anticipating the initial supply to last for several months, interest in the program far exceeded expectations – all of the donor milk was used within 48 hours!
The team now has weekly check-ins to ensure their supply of donor breast milk meets demand, typically having 20 to 30 100-mL bottles available at a time. Any postpartum infant with a medical necessity requiring supplementation, or any parent requesting supplementation, is a candidate for donor breast milk. This allows parents who want to remain exclusively breast milk feeding the option to provide their infant with supplementation if needed. Donor breast milk is no longer provided if formula is given as supplementation.
As a result of launching this new program, Valley’s exclusive breastfeeding rate has increased, as shown in the graph below. Valley’s lactation team looks forward to continued growth of the donor breast milk program in 2026 and beyond!
The Lasting Impact of Mentorship
The Valley Hospital's MIND (Mentors in Nursing Development) program supports new graduate nurses by pairing them with experienced mentors for nine months after their 16th week in the residency program. Mentors, who help guide personal and professional growth, are selected through an application, training session, and questionnaire to ensure a strong match with their mentees. Mentees meet with their mentors monthly during their first year to receive continuous guidance and support.
The MIND Mentorship Program is more than just a structured initiative – it’s a valuable support system that fosters personal and professional growth for both mentors and mentees. Through guidance, encouragement, and shared experiences, mentors help shape the future of nursing, while mentees gain the confidence and knowledge they need to succeed. For any nurse considering joining the program, whether as a mentor or mentee, the benefits are clear: strong relationships, career growth, and a supportive community dedicated to excellence in nursing.
What Our Nurses are Saying
“My experience as a mentor has really been a full-circle moment for me. I’ve been excited to share the tips and tricks I’ve learned during my time at Valley. I’ve had the privilege of learning from some amazing nurses, and I really enjoy the opportunity to pass down this knowledge to new resident nurses.”
- Maason Klemick, RN, Neuro ICU
“The emotional support from my mentor has been invaluable. He understands the stress and anxiety that comes with being a new grad nurse, so having someone who can relate to my experiences has been incredibly helpful.”
- Meiqi Xue, RN, 4Wa Cardiac Telemetry
TeamBirth: Improving Transparency at the Bedside
To help improve communication, teamwork, and shared decision-making for patients, families and their care teams throughout the birthing process, in 2025 The Valley Hospital’s Center for Childbirth implemented the TeamBirth program.
After learning about TeamBirth at a national conference, Maira de Leon, MSN, RNC-OB, C-EFM, Director of Inpatient Family Care Services, and her team researched how the program can help improve transparency and outcomes for patients and their families at Valley’s Center for Childbirth. Through close collaboration with the New Jersey Healthcare Quality Institute and Ariadne Labs – the organizations that lead the initiative – Valley officially launched the TeamBirth program at the hospital in September 2025.
The program centers around team huddles that include the patient, their family, and members of their care team, which can include nurses, physicians, midwives, or any other person involved in their care. The huddles allow for everyone to discuss the plan of care together, ensuring that all are in alignment and that the patient’s voice is heard throughout the birthing process. The patient can request a huddle at any time if they have a question or concern or would like to talk through a change in their plan. The plan of care is also written on a white board in the patient’s room so that it is visible to all who enter.
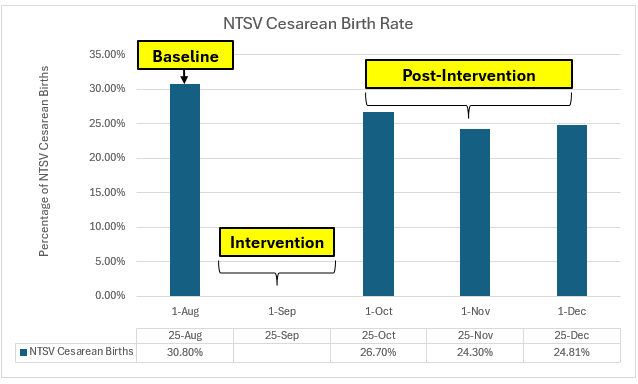
Since launching the program, Valley has seen an improvement in the NTSV cesarean birth rate at the Center for Childbirth, as shown in the graph below. This is the rate calculated for first-time pregnant patients (N = Nulliparous), greater than 37 weeks pregnant (T = Term), only delivering one infant (S = Singleton), and head down delivery (V = Vertex).
TeamBirth is just one of many ways Valley is involving patients and their families in their care to help foster open communication and improve outcomes.
Saying “Yes” to Meaningful, Patient-Centered Needs in Valley Hospice
Valley Hospice’s Hospice Spending Program is a discretionary fund used to support special, non-routine needs of hospice patients and families, above and beyond what is normally covered by hospice benefits. The goal is to enhance comfort, dignity, and quality of life, especially when a relatively small expense can make a big emotional or practical impact.
The Hospice Spending Program can be used for:
- Comfort or quality-of-life items (e.g., a small piece of equipment, a special blanket, hobby supplies, a printer so a patient can write or create)
- Practical support for families under significant stress (e.g., a limited amount of gift cards for groceries, gas, or basic necessities)
- Items or experiences that help the patient feel seen and valued (e.g., something related to a long-time interest, faith, or personal goal, as appropriate)
The Hospice Spending Program doesn’t replace or duplicate what Valley Hospice already covers (medications, DME, standard supplies) or to pay for large, ongoing household expenses. Rather, it is a targeted, one-time or short-term support when a team identifies an unmet need that fits the spirit of hospice: comfort, connection, and dignity at the end of life.
Typically, the process works like this:
- A team member (nurse, social worker, chaplain, home health aide, volunteer, etc.) identifies a need during visits.
- The need is discussed to ensure it’s appropriate, equitable, and within the program’s budget and guidelines.
- A request is submitted (often with a brief justification linked to patient/family goals of care) and approved.
- The item or support is purchased through the approved mechanism (e.g., agency purchase, gift card, etc.).
- The team documents the intervention in the record, including how it supports the patient’s comfort, coping, or quality of life, and keeps any required receipts.
At its heart, the Hospice Spending Program is about giving teams a tool to say “yes” to meaningful, patient-centered gestures – especially when time is short and the impact can be profound.
New Medicare Regulation: Hospice HOPE Documentation
This year, Valley Hospice’s nursing team prepared for and began implementation of the new Medicare Hospice HOPE (Hospice Outcomes & Patient Evaluation) documentation requirements, introduced by CMS as part of an updated quality and assessment framework for hospice care.
Under this regulation, hospices are required to complete standardized HOPE assessments at defined points in the patient’s stay, capturing information on symptom burden, functional status, safety, psychosocial needs, and caregiver support in a consistent and measurable way.
HOPE went into effect on October 1st, 2025; for nursing, this regulation represents a significant shift from traditional narrative-only documentation to a more structured, data-driven approach. HOPE responses directly support Medicare quality reporting, help demonstrate the value of hospice services, and provide comparable data across agencies nationwide.
Valley Hospice’s nursing team has focused on:
- Education and training: teaching nurses when HOPE is required, how to complete the tool accurately, and how it integrates into existing workflows
- Workflow alignment: building HOPE into the admission, routine visit, and recertification processes to minimize duplication and ensure timely completion
- Quality and compliance monitoring: reviewing charts for completion rates and accuracy, and providing real-time coaching and feedback
While the new HOPE regulation has added complexity to documentation, it has also strengthened the clinical clarity and consistency of our nursing assessments and enhanced communication within the interdisciplinary team. Our ongoing goal is to maintain full regulatory compliance while keeping the focus on what matters most: using HOPE not just as a form, but as a tool to guide compassionate, individualized, and high-quality hospice care.
Meditech Upgrade Showcases Multidisciplinary Collaboration

On November 9, 2025, Valley upgraded Meditech, its electronic medical record platform, to Meditech 2.2. This upgrade transitioned the Patient Care Services (PCS), Emergency Department (EDM), Surgical Services (SUR), and Oncology (ONC) modules to a web-optimized interface. The change was essential to improving mobility, increasing functionality, streamlining processes, and aligning the user interface experience across clinical areas.
Staff education and training were key to preparing employees. The education rollout, led by Lora Bognar, PhD, RN, ANP, NE-BC, NPD-BC, Director, Nursing Professional Development/Simulation Center, and Aimee Lukose, MBA, MSN, RN, Manager, Clinical Informatics, assigned training to all users of the PCS, EDM, SUR, and ONC Meditech modules, with opportunities to complete the training in their department or at a dedicated training space at an off-site location. A total of 1,041 nurses completed the training prior to the Meditech 2.2 go-live on November 9.
Immediately after go-live, employees were assisted via a Command Center, which was staffed by Information Systems team members (shown above), and at-the-elbow support. Tip sheets and other documentation available on Valley’s intranet further ensured a seamless transition to the new system.
The Meditech 2.2 upgrade showcased successful collaboration and partnership between Valley’s Nursing Professional Development, Clinical Informatics, and Information Systems teams. Together, the departments provided nursing staff with consistent information, reliable support, and, ultimately, an improved user experience.
