EMPIRICAL OUTCOMES focuses on demonstrating how structures and processes produce outcomes in the healthcare team, organization, and systems of care essential to a culture of excellence and innovation.
The Valley Hospital
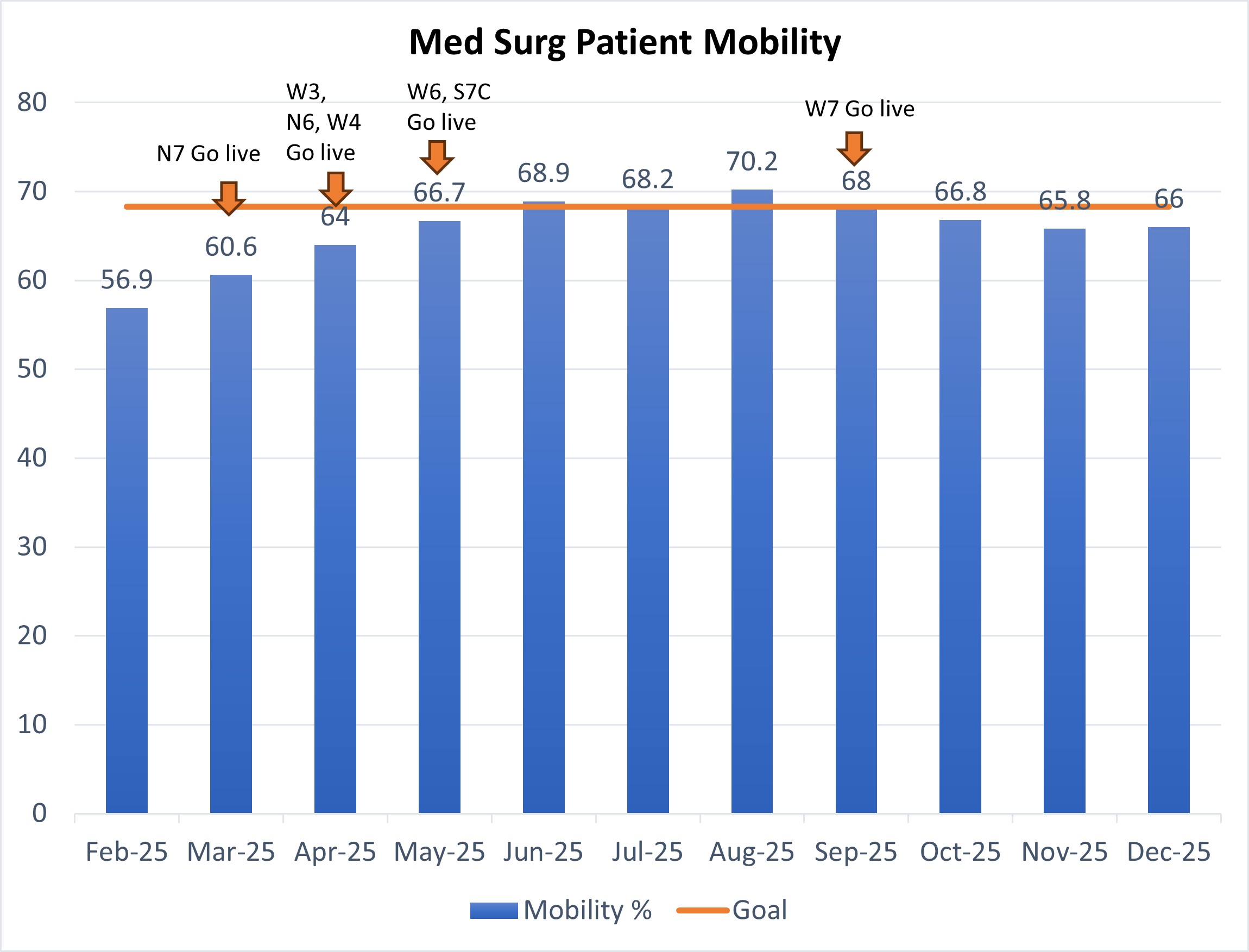
Impact of Nurse-Led Mobility Guidelines in Med-Surg Units
During acute illness and hospitalization, decline in mobility is common and has an outsized impact health, independence, and quality of life, especially among older adults. Loss of mobility is associated with increased length of ventilator days, increased length of hospital stays, and adverse outcomes during and following hospitalization, including falls, declines in activities of daily living (ADL), and nursing home placement. Despite its importance, loss of mobility is not a widely recognized outcome of hospital care. The team at Valley increased patient mobility on the med-surg units from 56.9% in February, 2025 to 66% in December, 2025. This 18% increase in mobility was attributed to introduction of the nurse-led mobility guidelines. Units included N6, N7, W3, W4, W5, W6, W7, and S7C.
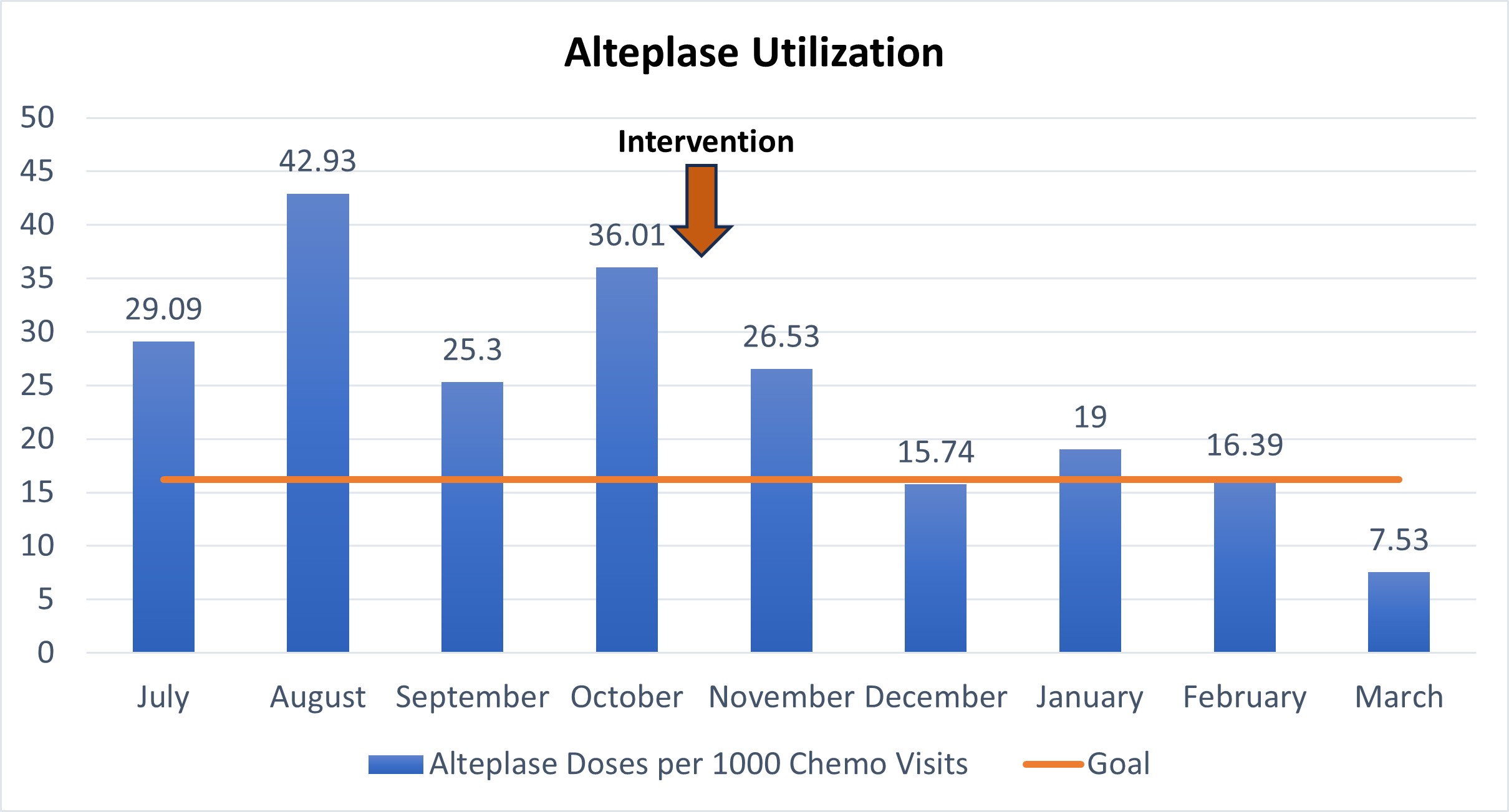
Alteplase Utilization in Outpatient Infusion
As a result of increased clotting in central venous access devices, such as ports or PICC lines, alteplase use in outpatient infusion increased markedly in 2025 over the prior year. Increased alteplase use is associated with delays in treatment initiation, increased anxiety and dissatisfaction of patients and caregivers, and increased cost. This project reduced the use of alteplase in outpatient infusion from 32.44 doses per 1,000 chemotherapy visits between July and September, 2024, to 14.31 doses. This 77% decrease in alteplase use was achieved by the end of first quarter 2025 as a result of nursing and physician education and enhanced fields for documentation in the EMR.
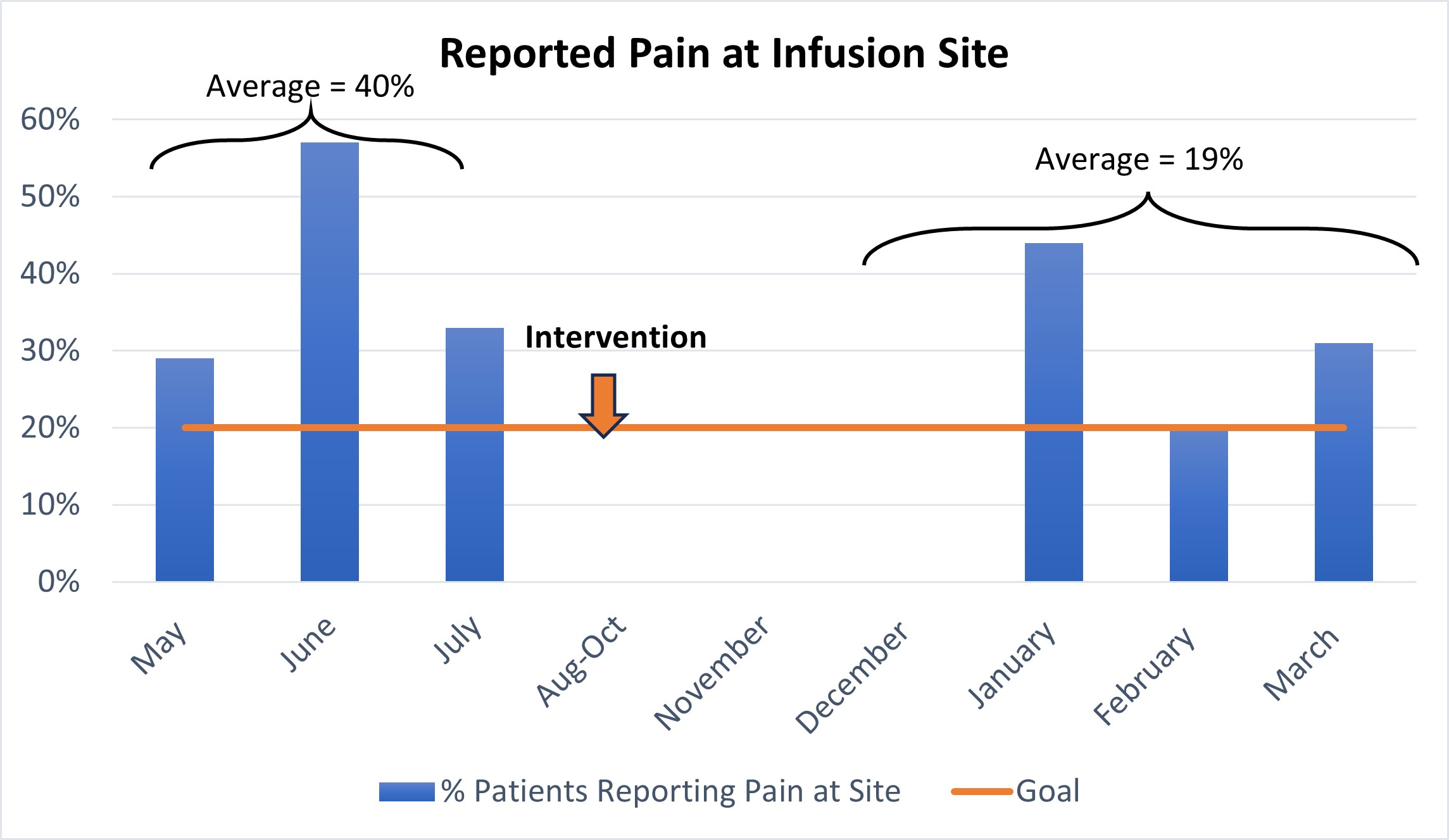
Decreasing Pain During Potassium Chloride Infusions on W6 Oncology
Infusion of intravenous potassium chloride (IV KCl) can cause pain at the infusion site for patients. Through a nurse’s submission of a clinical question to the Research Council at The Valley Hospital, it was determined that there is currently no standard or protocol for nurses to follow to prevent pain at the infusion site when administering IV KCl to patients. Nurses on W6 Oncology developed a protocol to standardize nursing practice and successfully reduced patient reported pain related to IV potassium infusion from an average of 40% (May-July 2024) to an average of 19% (January-March 2025).
Alarms Reduction Through a Rapid Improvement Event
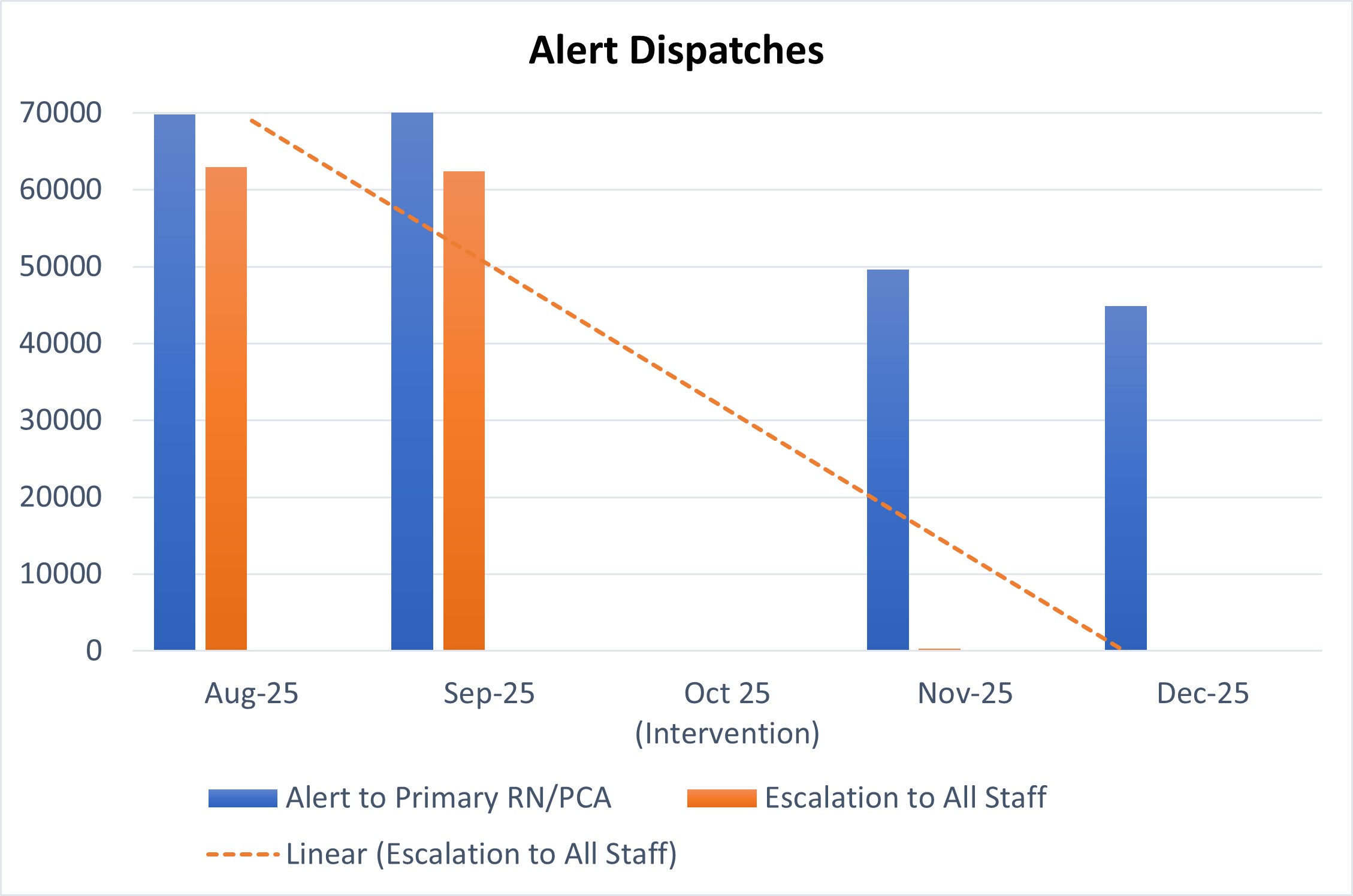
After a Rapid Improvement Event focused on alarm management, N4A Cardiac Telemetry was selected as the pilot unit to test alarm‑optimization strategies. The team eliminated the escalation of nurse call alerts to Vocera for all staff. Now, when a patient presses the call bell, the Connexall alert is sent only to the assigned RN and PCA, with no further escalation. This change reduced the total number of Connexall alerts sent through Vocera by 25% on the trial unit. The trial was expanded hospital‑wide in September and resulted in a 43% and 41% reduction in notifications to RNs and PCAs, respectively. Decreasing excessive alarm notifications helps staff to focus and respond to the most important alarms in a timely manner.
Reducing Central Line Associated Bloodstream Infections at TVH
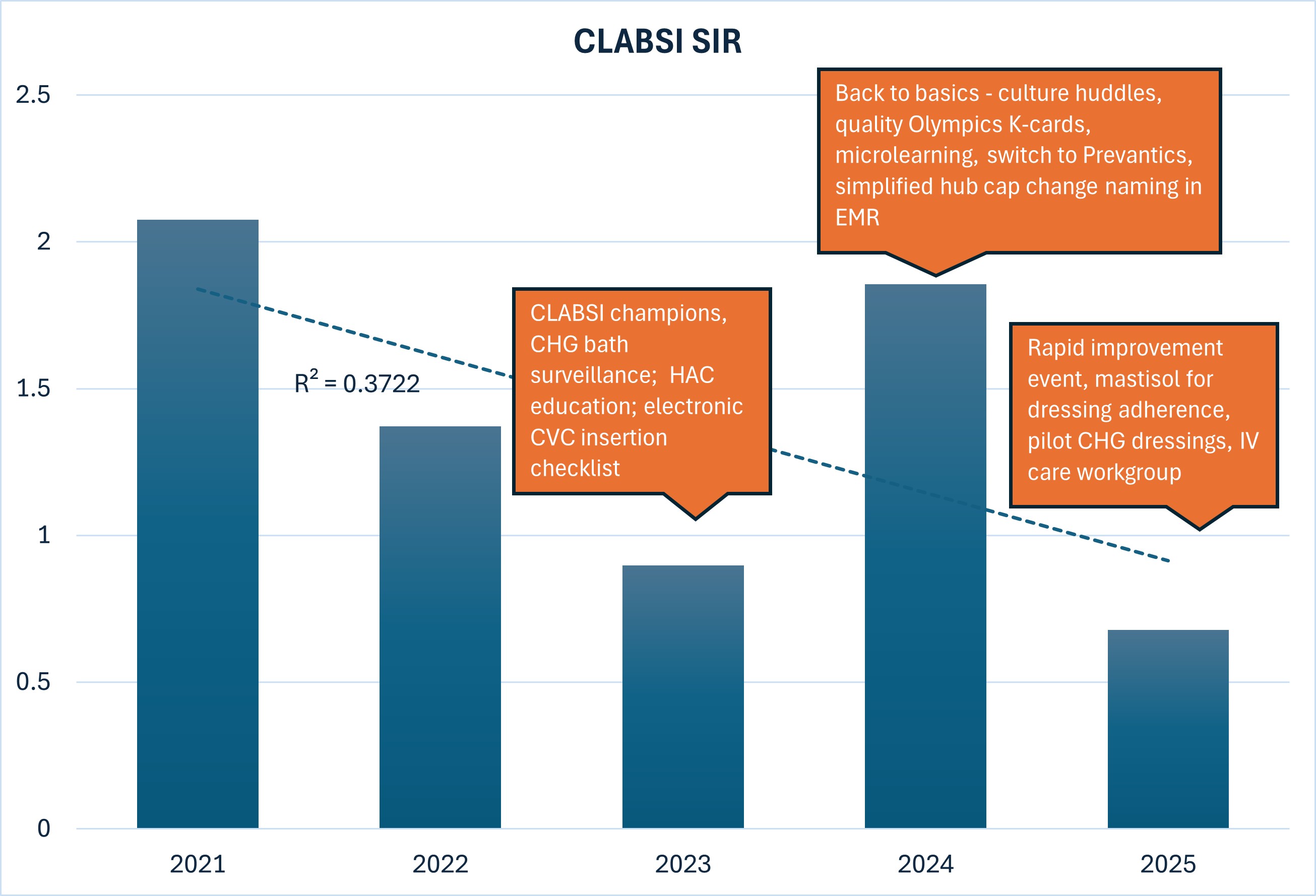
There has been continued progress in reducing Central Line-Associated Bloodstream Infections (CLABSIs), an important indicator of nursing excellence. The Standardized Infection Ratio (SIR) compares the number of infections we have to the number expected nationally; a SIR below 1.0 means fewer infections than predicted and reflects strong, consistent nursing practice.
Through focused interventions – such as improved CHG bathing practices, electronic insertion checklists, enhanced education, and strengthened maintenance routines – nurses, the HAI Taskforce, and Infection Prevention have worked together to improve central line safety. Lower CLABSI rates positively influence outcomes in programs like Leapfrog and Medicare Value Based Purchasing, where infection prevention is a key measure of quality.
While this trend shows meaningful improvement, ongoing vigilance and continued adherence to best practices remain essential. This chart represents a strong movement in the right direction and highlights the impact of nursing driven quality efforts.
Patient Experience (Press Ganey) Scores for TVH Inpatient Areas
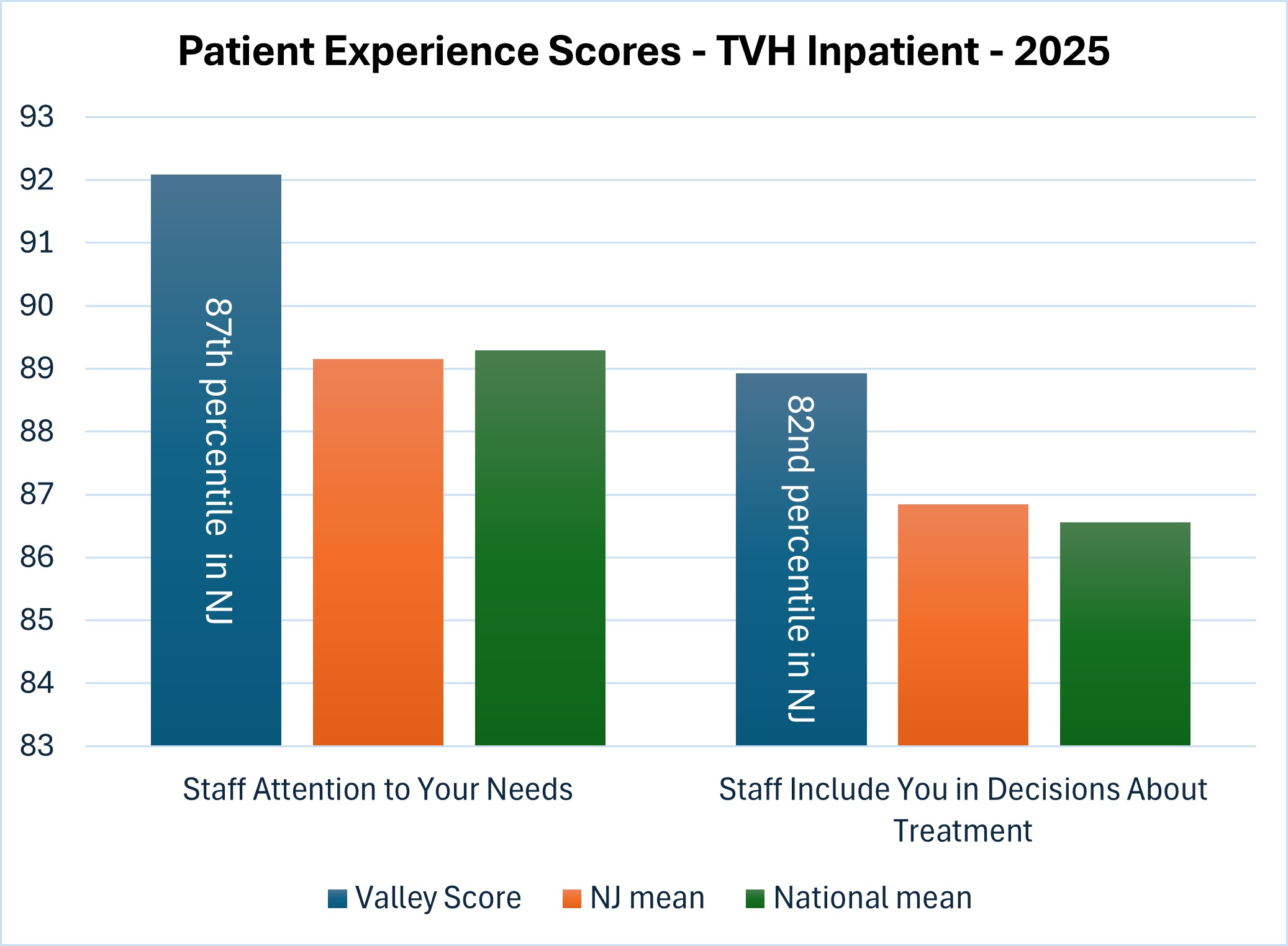
Valley nurses led the way on patient experience surveys, demonstrating 87th percentile ranking for “Staff Attention to Your Needs” and 82nd percentile ranking for “Staff Include You in Decisions About Treatment” as compared to other New Jersey facilities. This demonstrates high quality, patient-centered nursing practice.
Patient Experience (Press Ganey) Scores for TVH Ambulatory Surgical Care
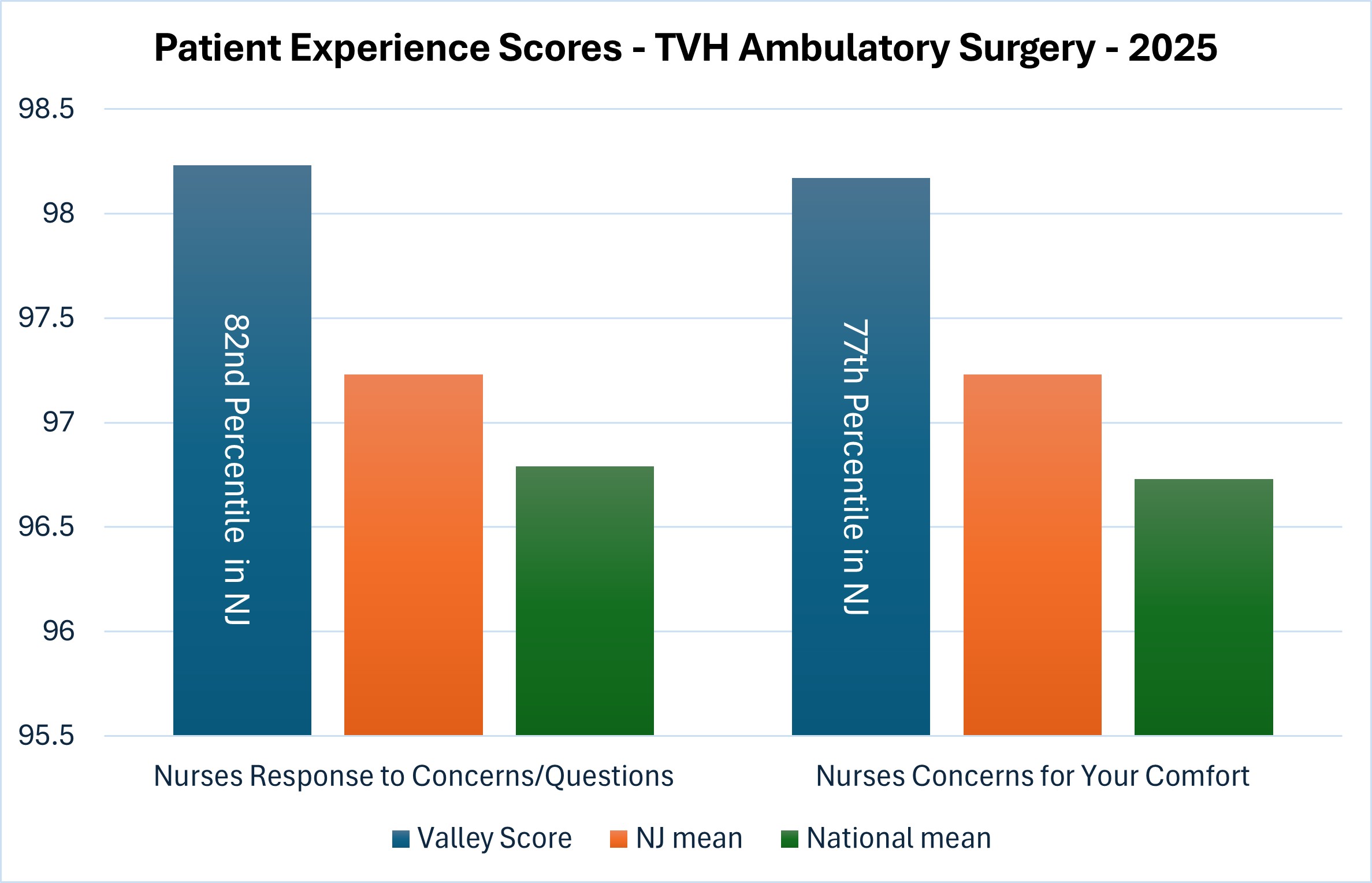
Valley nurses continue to demonstrate exemplary practice in ambulatory surgery, as reflected for 82nd percentile ranking for “Nurses Response to Concerns/Questions” and 77th percentile ranking for “Nurses Concerns for Your Comfort” when compared to other New Jersey facilities.
Valley Medical Group
Patient Experience (Press Ganey) Scores for VMG
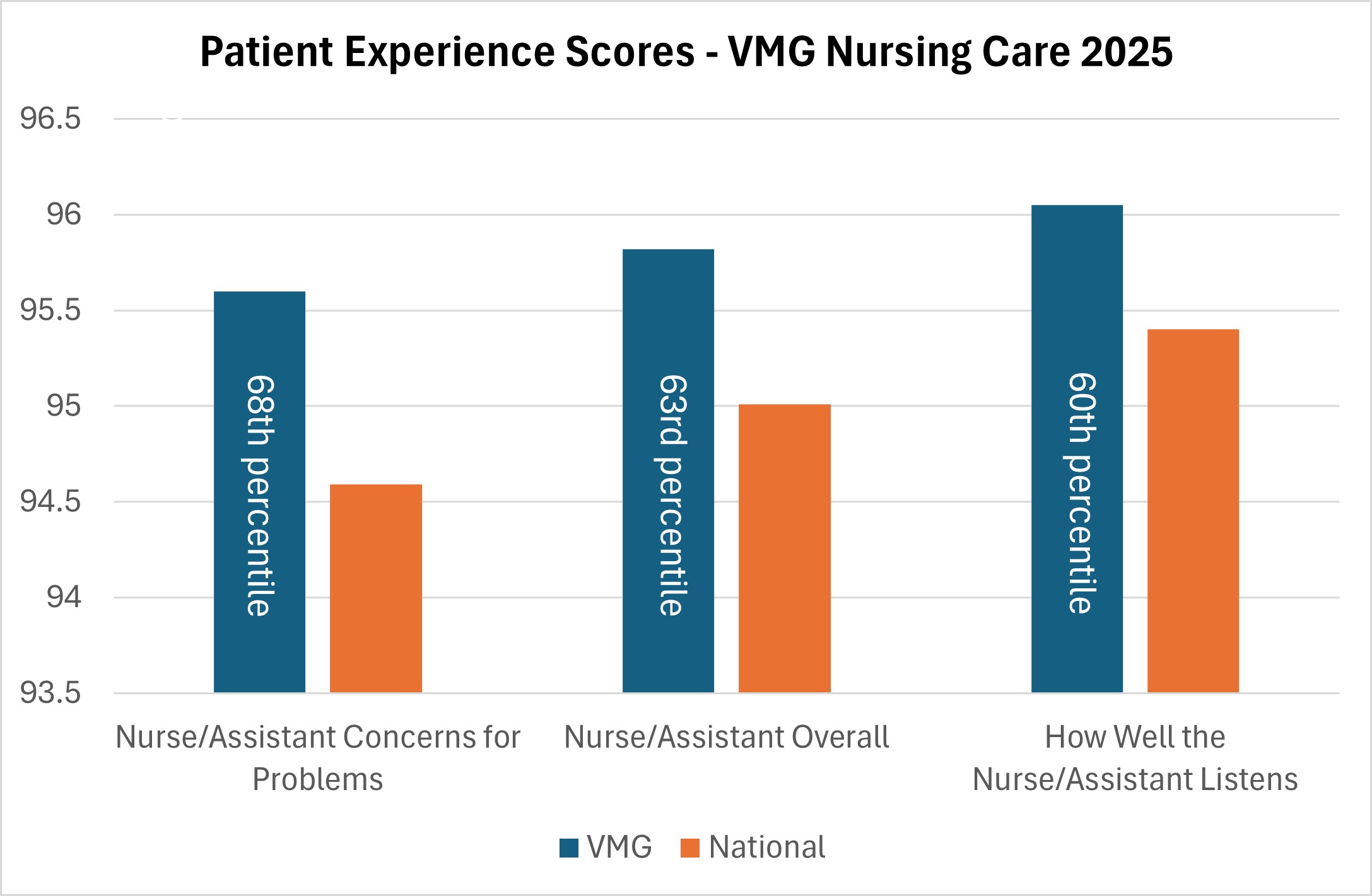
VMG nurses and assistants outperformed patient experience scores nationwide related to “Nurse/Assistant Concerns for Problems,” “Nurse/Assistant Overall,” and “How Well the Nurse/Assistant Listens,” reflecting high quality and patient-centric nursing practice.
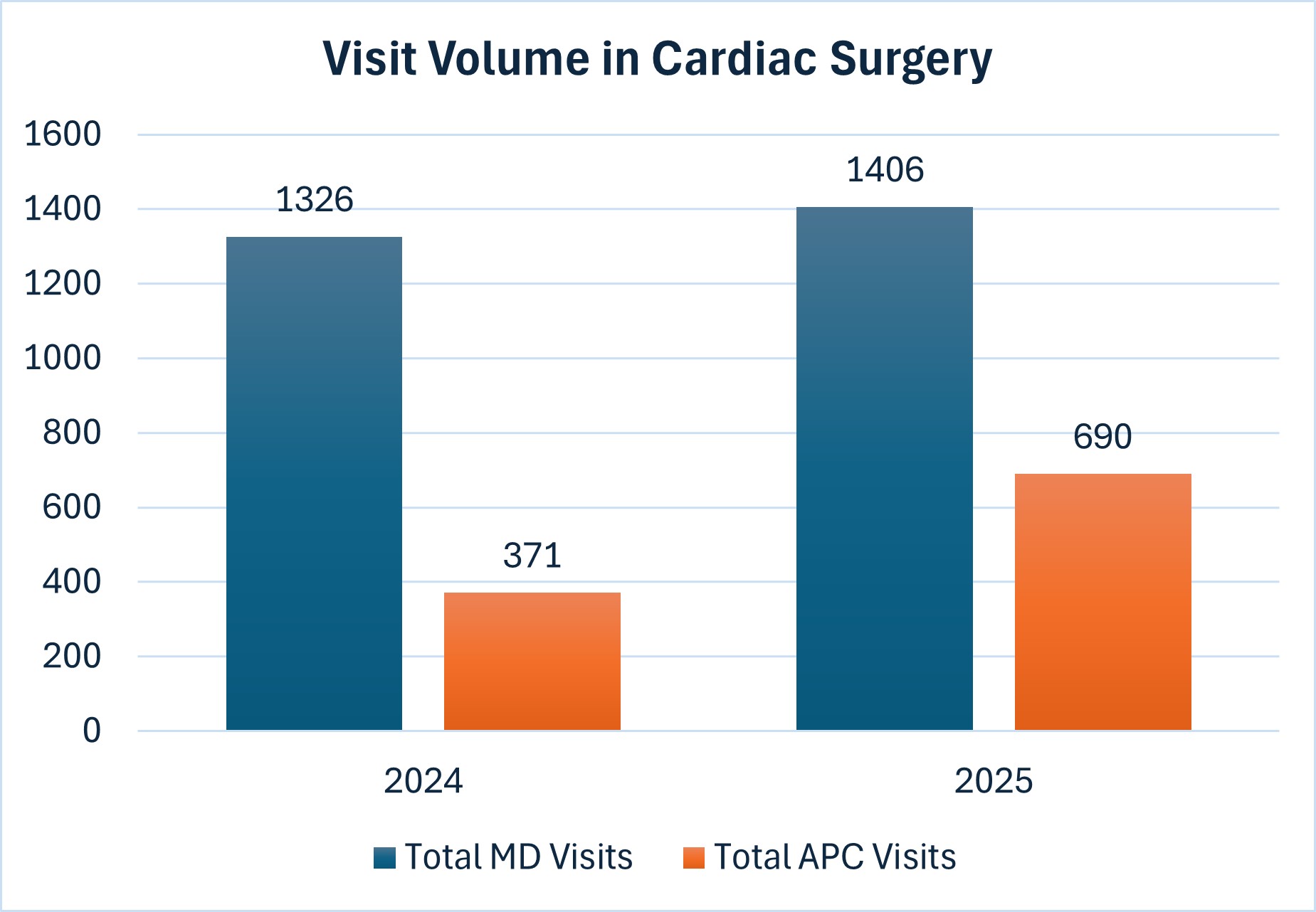
Increasing Patient Access in Cardiac Surgery Using APCs to Top of License
The implementation of an Advanced Practice Clinician (APC)-driven care model significantly increased patient access, reducing wait times for cardiac surgery appointments and supporting year over year visit growth by 25%. By practicing at the top of their license, APCs effectively managed lower acuity and follow up patients, enabling physicians to accommodate more new and complex cases. This collaborative model not only improved operational efficiency and patient experience but also strengthened the overall quality of care within the service line.
Valley Home Care / Valley Hospice
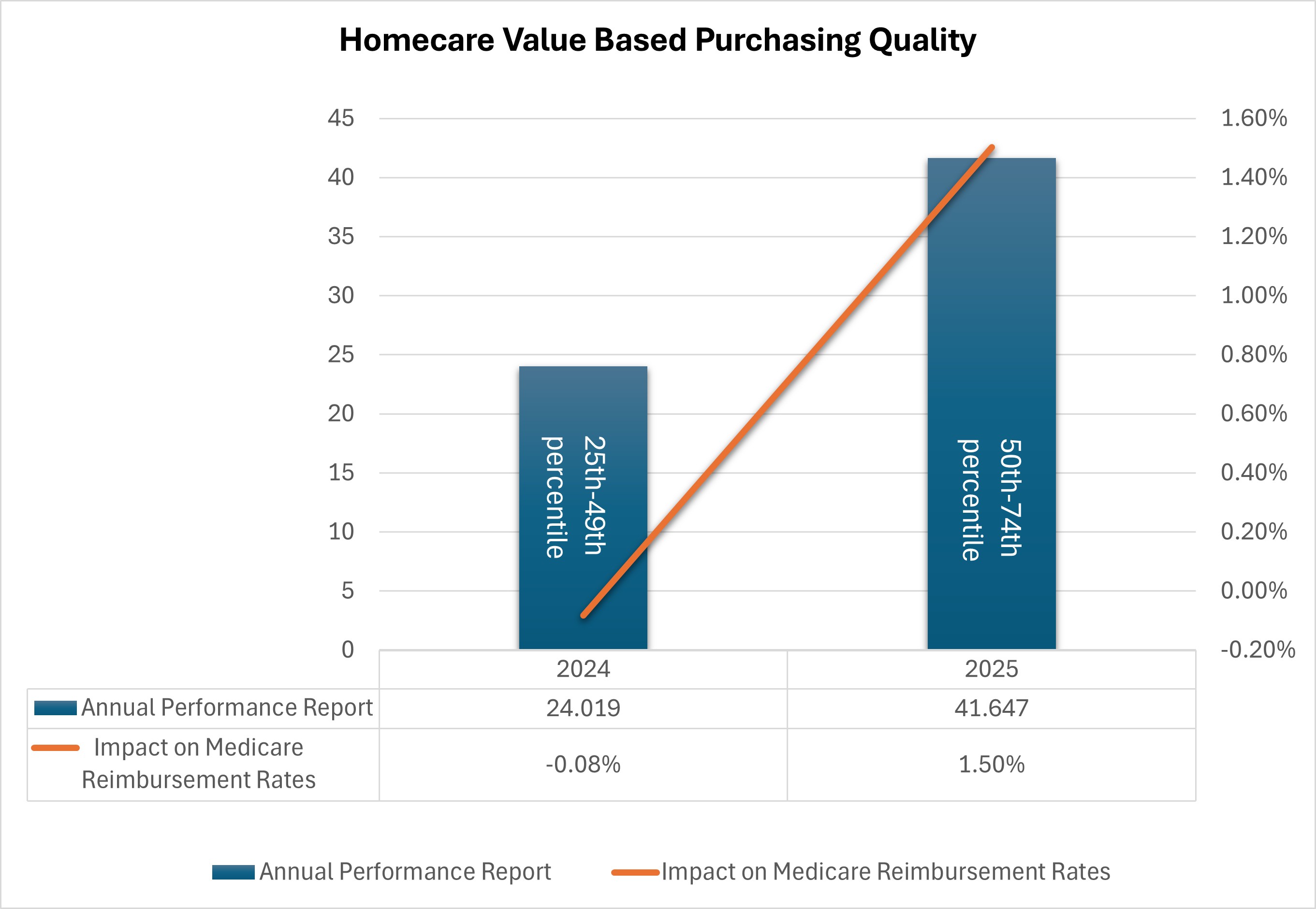
Value-Based Purchasing Quality in Valley Home Care
In 2025, Valley Home Care achieved a significant improvement in its Total Performance Score under the CMS Home Health Value-Based Purchasing program, reflecting measurable gains in patient outcomes, safety, and overall quality. Our performance advanced from a lower national tier to an above-average tier, demonstrating the impact of consistent, high-quality nursing practice, documentation accuracy and care coordination. These improvements mean that more patients are benefiting from safer transitions, improved symptom control, and stronger recovery at home. This progress also resulted in a positive Medicare payment adjustment, which helps support continued investment in staff education, quality initiatives, and resources that further strengthen patient services.
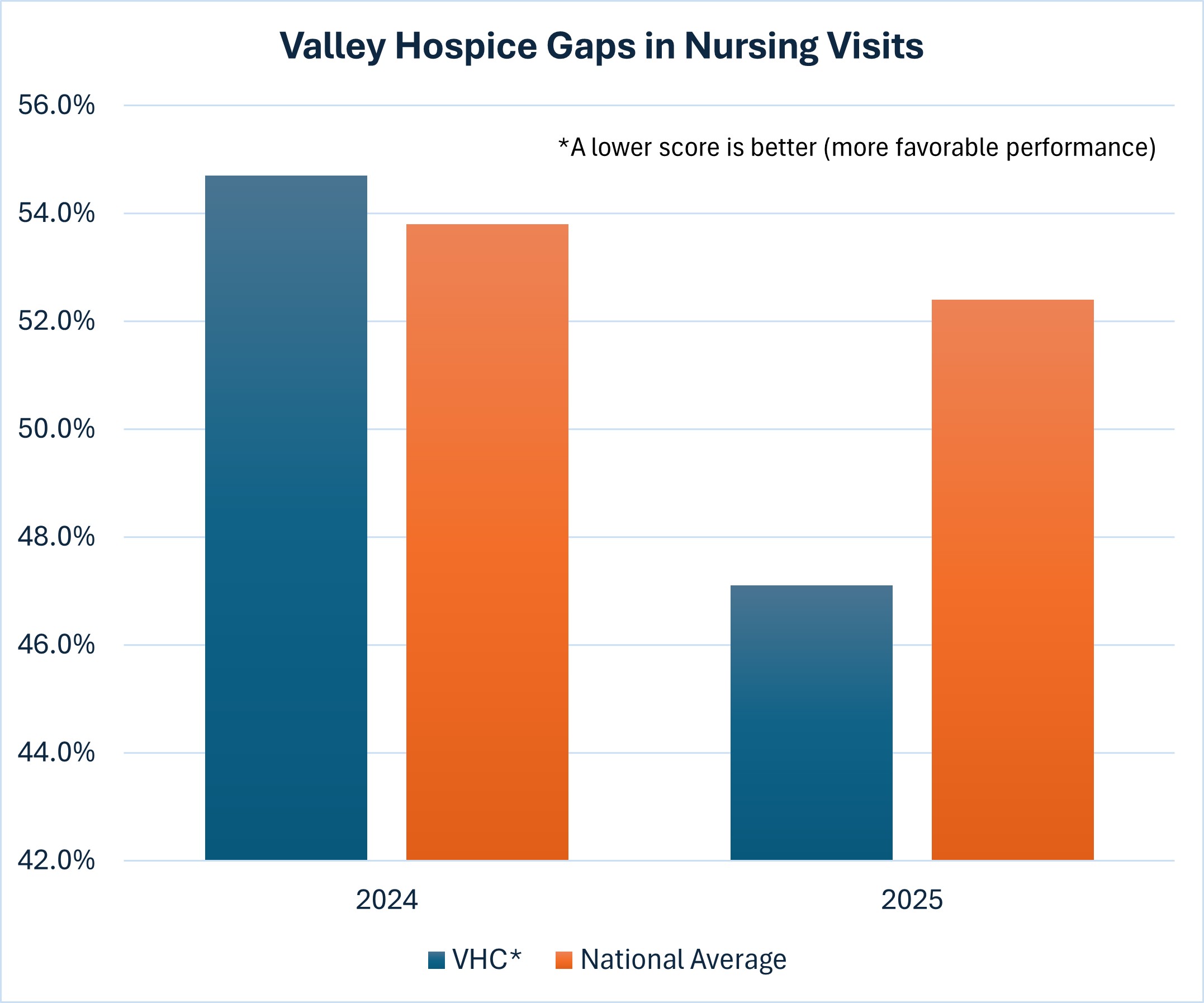
Reducing Gaps in Nursing Care During Valley Hospice Visits
In 2025, Valley Hospice demonstrated meaningful improvement in continuity of nursing services, as reflected by a reduction in gaps between scheduled nursing visits. For this measure, a lower score reflects better performance. Our performance improved from slightly above the national average in 2024 to well below the national average in 2025, indicating stronger reliability in visit scheduling and follow-through. Fewer gaps in nursing visits mean that patients and families are receiving more consistent clinical support, symptom management, and emotional care during a highly vulnerable time. This improvement reflects the commitment of our hospice nursing team to timely presence, proactive coordination, and maintaining continuity of care for patients at the end of life.