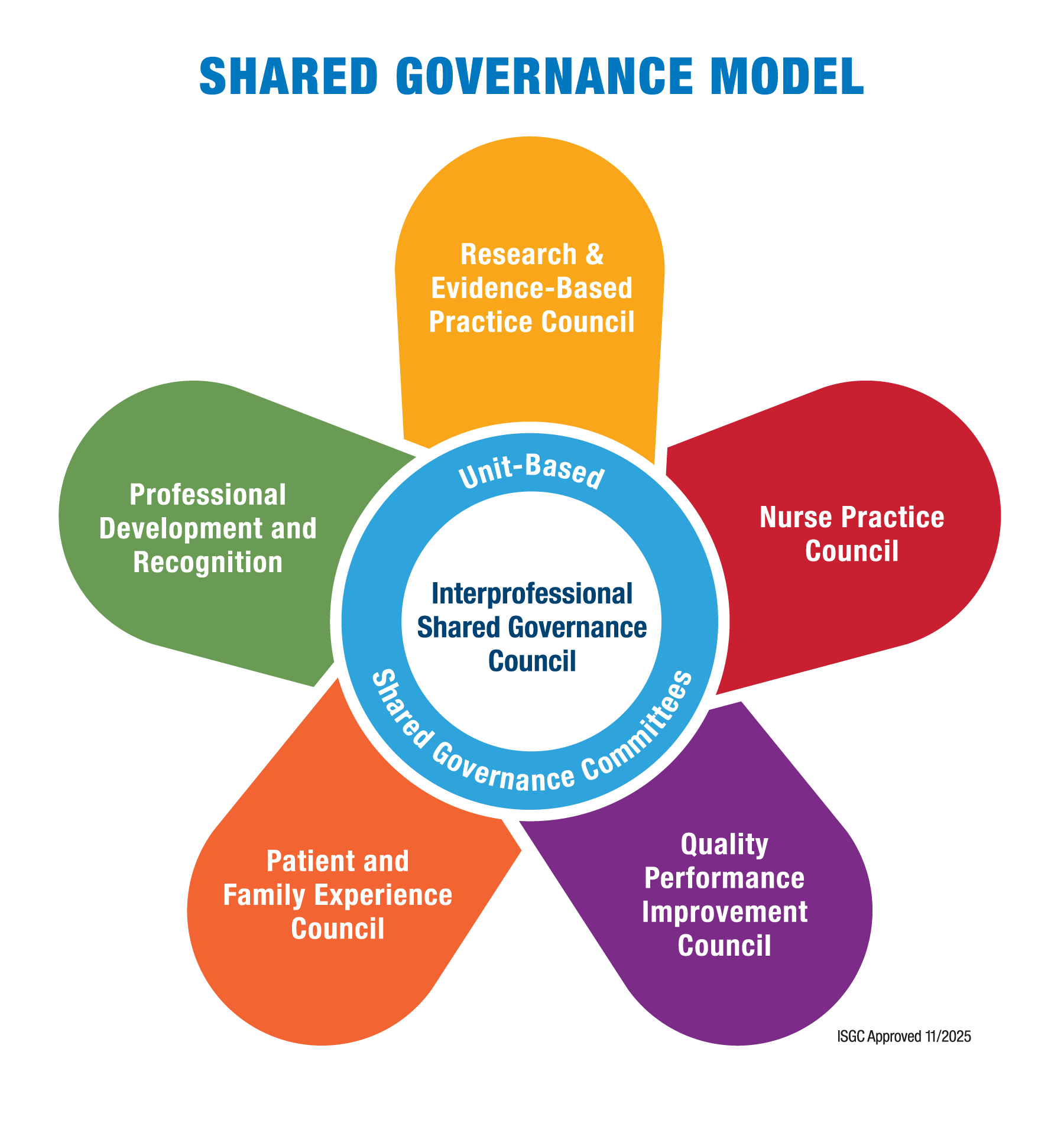
EXEMPLARY PROFESSIONAL PRACTICE focuses on how nurses throughout the organization are involved in shared governance and shared decision-making, and explores how interprofessional collaboration promotes quality excellence in a culture of safety.
The Valley Hospital Earns Recognition for Providing Age-Friendly Care
 In July 2025, The Valley Hospital was proud to earn recognition as an Age-Friendly Health System Participant for its ongoing commitment to delivering safe, reliable care to aging patients.
In July 2025, The Valley Hospital was proud to earn recognition as an Age-Friendly Health System Participant for its ongoing commitment to delivering safe, reliable care to aging patients.
The Age-Friendly Health Systems designation, an initiative of The John A. Hartford Foundation and the Institute for Healthcare Improvement, in partnership with the American Hospital Association and the Catholic Health Association of the United States, recognizes health systems that provide exceptional care in meeting the unique needs of older adults.
The initiative is based on a series of practices focused on addressing four essential elements of care for older patients (known as the 4Ms):
- What Matters: Know and align care with each older adult’s specific health outcome goals and care preferences, including, but not limited to, end-of-life care, and across settings of care.
- Medication: If medication is necessary, use age-friendly medications that do not interfere with What Matters to the older adult, Mobility or Mentation across settings of care.
- Mentation: Prevent, identify, treat and manage dementia, depression and delirium across settings of care.
- Mobility: Ensure that older adults move safely every day in order to maintain function and do What Matters.
By embedding the 4Ms into routine practice, Valley is strengthening care coordination, reducing preventable complications, and ensuring that aging patients receive safe, high-quality care that is aligned with what matters most to them.
Leading the Way in Workplace Violence Prevention: Nursing Driving a Culture of Safety
Workplace violence remains a significant risk in healthcare, with frontline staff experiencing nonfatal violence at rates far higher than most other professions. These incidents contribute to emotional distress, burnout, and potential impacts on patient care. Recognizing that a safe practice environment is essential to clinical excellence, nursing at The Valley Hospital has taken a leading role in prevention, education, and system-level improvements.
Crisis Prevention Institute (CPI)
While all employees complete annual required virtual workplace violence prevention training, Valley’s Nursing Professional Development and Simulation Center recognized an opportunity to further strengthen frontline preparedness through immersive, hands-on learning
Lora Bognar, PhD, RN, ANP, NE-BC, NPD-BC, Director of the Nursing Professional Development and Simulation Center, led a partnership with the CPI to introduce hands-on training through CPI’s Nonviolent Crisis Intervention® program. This program equips nurses and frontline staff with practical, nonviolent de-escalation and crisis intervention techniques. To date, more than 775 employees have completed CPI training, and ten employees have pursued certification as CPI trainers, strengthening internal expertise and sustainability. Nursing champions Virginia Wydak, BSN,RN, HN-BC, Joseph Ballesteros, BSN, RN, PCCN, and Lauren Piech DNP, MPH, RN, NI-BC, NEA-BC, HN-BC, played key roles in advancing the initiative.
Workplace Violence Algorithm
Nursing leadership also extended into system redesign. After frontline staff raised concerns about disruptive visitor behavior, nurses elevated these issues to leadership, prompting the creation of a multidisciplinary workgroup to improve visitor management. Nurses were active contributors in developing a standardized Workplace Violence Algorithm for non-patients. Based on staff feedback, updates included expanded visitation hours, a streamlined overnight visitor approval process, clear code-of-conduct signage, and the introduction of the algorithm to guide staff when disruptive behavior occurs.
Broset Violence Checklist
Moreover, in 2025, nurses led implementation of the Broset Violence Checklist, an evidence-based tool that identifies patients at risk for aggressive behavior within 24 hours. Piloted in the Emergency Department and implemented across all clinical areas on May 1, 2025, the assessment is completed by nurses at admission and every 12 hours, with results displayed on digital door signage and included in handoff communication to promote team awareness and a safer care environment.
Learning Strategies to Beat Burnout and Boost Motivation
Valley’s organizational partnership across departments was highlighted in 2025 when the Patient Experience Department sponsored an event to support clinical staff well-being and performance. In December 2025, Valley Home Care staff attended a special session with Dan Catuccio, a physical therapist and healthcare social media content creator known for his engaging talks on reducing burnout, improving documentation, and finding motivation in the field.
More than 150 homecare clinical staff attended the event, both in person and virtually. The high turnout reflected responsiveness to the needs of frontline nurses, as burnout, motivation, and documentation challenges are key issues often identified through shared governance councils, staff feedback, and engagement surveys. Providing this education signaled that nurses have a voice in shaping professional development priorities.
By prioritizing burnout prevention and resilience, Valley invested in nurses’ well-being – an essential driver in quality outcomes and excellence in care – and advanced a culture of safety throughout the organization.

Valley Welcomes Two International Nurses
In 2025, Valley was proud to welcome two international nurses to the nursing staff – Michelle Samontanez, BSN, RN, and Gladys Barcelona, MSN, RN.
In response to the national nursing shortage, Valley partnered with Connetics USA, an international nurse recruitment agency, to search for qualified nurses to join the organization. After an extensive interview process, Valley hired and onboarded Michelle to the CSICU team in June and Gladys to the W4A Cardiac team in August.
Michelle, who is from the UK, and Gladys, who joined from the Philippines, attended Valley’s comprehensive nursing orientation program. They also received additional one-on-one training to learn how to use various technologies, including Meditech and specific hospital equipment.
Michelle and Gladys have been wonderful additions to the nursing teams, and we look forward to continuing our recruitment efforts to hire more international nurses in the future!

Mentorship Across Disciplines: Valley Nurses Guide the Next Generation of Physicians
In 2025, Valley’s Nurse Buddy and Resident Peer Mentoring Program was launched to bring nurses into a shared mentoring and support role with residents enrolled in the Graduate Medical Education Program. The initiative pairs all medical residents (as mentees) with self-selected volunteer nurses and advanced practice providers, as well as senior residents, within Valley who are eager to collaborate and help navigate the hospital system.
This collaboration positions nurses as equal contributors to training and professional development. In this way, nurses are not solely supporting clinical tasks; they are actively mentoring medical residents, helping them understand workflows, patient care processes, and the healthcare system.
By selecting nurses as mentors, the program recognizes their unique knowledge of patient care, hospital operations, and team coordination, reinforcing their value within the interprofessional team. These early relationships between medical residents and nurses promote open communication, reduce hierarchical barriers, and foster trust, leading to improved team-based care and patient safety.
Nurse-Led Interdisciplinary Collaboration Strengthens Pressure Injury Prevention
In 2025, nurses from the Wound and Ostomy Center (WOC) identified a hospital-acquired pressure injury (HAPI) and, through shared governance, came together to conduct a comprehensive root cause analysis. This nurse-led review revealed that the patient was clinically malnourished, increasing their vulnerability to skin breakdown.
Rather than addressing the issue in isolation, the WOC nurses partnered with the Clinical and Community Nutrition Department to identify opportunities to improve care and prevent future harm. This nursing-initiated collaboration led to meaningful practice changes that strengthened patient safety and quality outcomes across the organization.
Through this partnership, new interdisciplinary workflows were developed to support earlier identification and intervention for at-risk patients. Nutrition now reviews the WOC team’s SV Pressure Injury Prevention (PIP) Surveillance Board daily as part of its high-risk nutrition-leveling process. This shared visibility allows the Nutrition Department providers to proactively identify patients who may be experiencing nutritional deficiencies and intervene sooner. At the same time, the WOC team reviews the Nutrition Department’s malnutrition tracking boards and the nutritional supplements provided to patients, creating a two-way flow of information that supports more coordinated, effective care.
Both disciplines now consult with one another when patients may benefit from specialized wound or nutritional interventions, reinforcing a team-based approach to care planning. To further strengthen this collaboration, the Nutrition Department began attending the Pressure Injury Task Force meetings, supporting ongoing communication, shared learning, and continuous improvement focused on patient safety.
Building on this success, the Nutrition Department has also begun meeting with critical care providers to discuss nutrition needs for high-risk patients and further coordinate care across settings.
This initiative highlights how nurses, empowered through shared governance, lead meaningful system-level improvements. By fostering open communication and strong interprofessional partnerships, this work underscores the essential role of collaborative care in preventing harm and promoting safe, high-quality patient outcomes.
The Right Alert, at the Right Time: Nurses Lead System Redesign to Advance Safety and Workflow
The Valley Hospital’s transition to its new building in 2024 introduced advanced technologies designed to enhance patient care. However, the increased use of technology also resulted in a significant rise in bedside alarm notifications. Frontline nurses quickly identified that the growing volume of alerts was contributing to alarm fatigue, workflow disruption, and cognitive burden. Through Valley’s shared governance structure, nurses elevated this concern and advocated for action.
In 2025, the Performance Improvement Team partnered with bedside nurses to lead a Rapid Improvement Event (RIE), a focused initiative that brings key stakeholders together to analyze processes, identify root causes, and implement improvements. This nurse-driven effort demonstrated shared decision-making by enabling frontline nurses to influence system-level changes affecting patient safety and care delivery.
Alarm fatigue is a recognized patient safety risk. Frequent, non-actionable alarms from monitors, infusion pumps, and other technologies can desensitize caregivers and potentially delay responses to critical alerts. Excessive alarms also contribute to stress, cognitive overload, and burnout. Nurses leading this initiative recognized that addressing alarm fatigue was essential to ensuring timely recognition of patient changes, supporting nurse well-being, and maintaining a culture of safety.
Using the SIPOC framework (Suppliers, Inputs, Process, Outputs, Customers), the team identified key stakeholders across the continuum of care, including the Emergency Department, Family Care Services, Medical-Surgical units, Critical Care, and Same Day Services. Digital Health Informatics nurses and Information Systems analysts partnered with the clinical team to align technical solutions with frontline needs.
Bedside nurses highlighted practical concerns, such as identical alarm tones representing different levels of urgency (e.g., stretcher and bed warmer alerts sharing the same sound). Information Systems partners evaluated feasibility and implemented system adjustments.
Following implementation, nurses tested the changes in practice and provided ongoing feedback to refine the system. The pilot began on North 4A: Cardiac/Telemetry Step Down Unit and was later expanded across clinical areas, guided by the principle of ensuring the right alert reaches the right caregiver at the right time.
The initiative resulted in a 36% reduction in Vocera alert dispatches to primary nurses and patient care assistants and a decrease in average Connexall messages per shift from 5 to 3.25 per nurse. Reducing unnecessary alarms improved focus, decreased cognitive overload, and allowed nurses more time for meaningful patient interaction - reinforcing that technology should support, not overwhelm, the caregiver.
Shared Governance Recruitment Fair
In 2025, the Shared Governance Recruitment Fair and the beloved annual Nurses Week Basket Raffle joined forces to create a fun and lively event!
The Nurses Week Basket Raffle featured more than 40 baskets, each one carefully curated, artfully arranged, and generously donated from departments across Valley Health System. As attendees perused the basket offerings, they also had the chance to learn all about shared governance at The Valley Hospital and how they could become a council member.
All in all, the day was a tremendous success as the shared governance councils were thrilled to recruit nine new members, and more than $8,000 was raised via the basket raffle to support two great causes: Medical Missions and The Valley Hospital Vibe events.
New Valley Initiatives Lead to Increased Transparency and Improved Patient Satisfaction
In 2025, Valley launched several new initiatives aimed at increasing transparency, helping to drive improvements in patient satisfaction scores.
What Matters Most Initiative
As part of the Institute for Healthcare Improvement’s Age-Friendly Care movement, in 2024, Valley Home Care and Valley Hospice began tailoring care plans for our aging patients based on how they answered the following question: “What matters most to you today?” Due to their success, Lynnelle Tampac, BSN, RN-BC, HNB-BC, Manager, and Kelly Kennedy, MSN, RN-BC, NP-C, Advanced Practice Nurse, decided to pilot the initiative on The Valley Hospital’s North 7A Geriatric Pulmonary inpatient unit. The unit saw a notable increase in their patient satisfaction scores and, as a result, the What Matters Most initiative was rolled out hospital-wide in 2025.
As part of the initiative, twice each day, nurses ask patients what matters most to them and document the response in Meditech. This information automatically populates onto a virtual whiteboard in the patient’s room, creating a transparent and highly visible reminder of the patient’s goals and preferences.
By incorporating What Matters Most discussions into their workflow, nurses and other members of the care team are able to tailor care plans that reflect patients’ personal wishes – whether that means prioritizing comfort, mobility, social connections, or treatment preferences. Feedback from both patients and staff has been overwhelmingly positive, underscoring the power of active listening and shared decision-making in improving health outcomes and overall satisfaction.
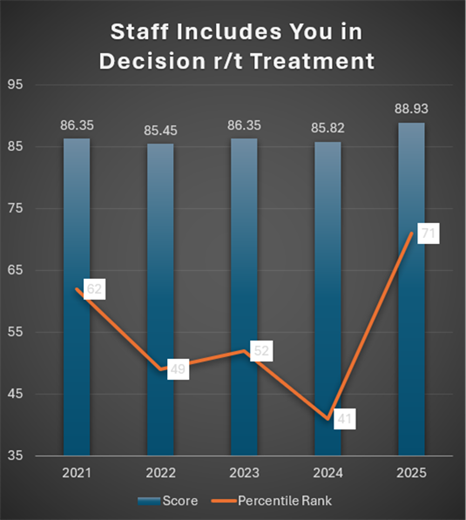
The graph below shows Valley’s inpatient score year after year for the metric, Staff Includes You in Decision Related to Treatment. This shows a significant increase for 2025 for both the score and percentile rank.
Emergency Department Wait-Time Tracker
With patient volumes continuing to rise, Valley’s Emergency Department (ED) sought new ways to improve communication and transparency for patients and their families. One of the most common concerns expressed by patients in the waiting area was uncertainty about how long they might need to wait.
To address this, in May 2025, the ED implemented a wait-time tracker board located prominently in the waiting area. Displayed on a large monitor, the board provides real-time insights into ED activity, including a color-coded visual of how busy the ED is at that time, the number of patients currently being treated, and estimated wait times. By offering a clear view of what is happening in the ED, the board helps set expectations and keeps patients well-informed during their visit.
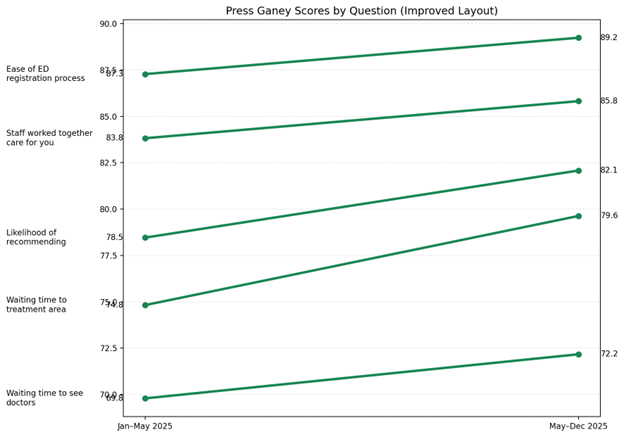
Front-line nurses and staff played a key role in developing the wait-time tracker board, ensuring the information presented is both meaningful and helpful for patients. As the graph below shows, since implementation last May, the ED has seen an increase in patient satisfaction scores in five different areas, demonstrating the positive impact that clear communication and transparency can have on the patient experience.
Perioperative Tracker Boards
In 2025, Valley introduced perioperative tracker boards to help improve communication and transparency for families and visitors waiting during a loved one’s surgery. The idea originated from feedback shared through the hospital’s Patient and Family Experience Council (PFEC), where members highlighted a common concern among visitors in the surgical waiting area: uncertainty about where their family member was in the surgical process.
Hospital leaders and perioperative staff met to explore ways to address this need and were inspired by the Emergency Department’s wait-time tracker board, which had successfully improved communication with patients. The team set out to create a similar tool for the surgical waiting area that would be easy to understand and provide timely updates for families.
The resulting perioperative tracker board displays real-time updates pulled directly from Meditech onto a monitor in the waiting area. Using patient initials for privacy, the board shows key milestones in the surgical journey, including the time they were admitted, when they entered the operating room, and when they moved to the recovery area. This information helps families better understand the progress of their loved one’s procedure.
Leader Rounding
Last year, Valley made leader rounding a key initiative to strengthen communication with patients and families and improve the overall care experience. The effort gained momentum after 12 members of nursing leadership attended a Press Ganey conference, where leader rounding was highlighted as one of the most effective ways to proactively address patient concerns and improve satisfaction.
Leader rounding encourages nursing leadership, including charge nurses, managers, directors, and other clinical leaders, to regularly visit patients and their families at the bedside. During these interactions, leaders ask targeted questions, listen to feedback, and address concerns in real time. These conversations often include asking patients what matters most to them during their stay, reinforcing Valley’s commitment to patient-centered care.
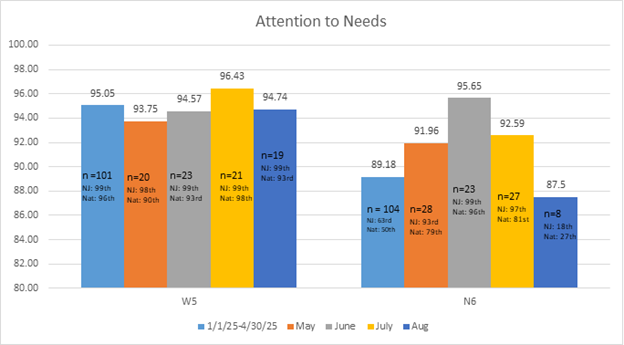
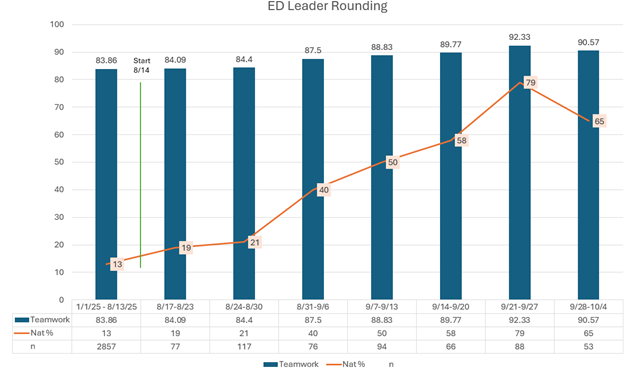
In May 2025, Brianne de la Rosa, BSN, RN, HN-BC, Manager, North 6A Neurology, and Jeanne Wilson, MSN, RN, CCRN, Manager, West 5A Bariatrics, piloted the initiative on their units with encouraging results as shown in the graph below. Both units saw a decrease in complaints and an increase in patient satisfaction scores for the question focusing on Attention to Needs. Based on this success, leader rounding was implemented hospital-wide, including in the Emergency Department (ED). As illustrated in the graph below, since implementation, the ED has seen a notable increase in patient satisfaction scores and percentile rank for the question focusing on Teamwork.
Each unit’s clinical shift supervisor, manager, and advanced practice provider round on a group of patients daily, ensuring that all 36 patients per unit are reached using the process that works best for their unit’s workflow. To keep the focus on meaningful patient interactions rather than documentation, the process was intentionally simplified. Leaders simply confirm that rounds were completed, emphasizing that the most important aspect of the initiative is the conversation taking place.